By Lucy Shaw, MBA, Author, Consultant, Transformative Life Coach for HeartWorks4U
 As Breast Cancer Awareness Month comes to an end, most of us must admit to knowing something about the radical bilateral mastectomy performed on the 38-year-old Angelina Jolie last May, if only by reading magazine headlines while standing in line at the grocery store. This sensational story not only underscores the ways our healthcare system can support women—famous or not—but at a deeper level, it highlights how it can fail to provide women with the kind of informed choices that can dramatically impact their lives. A new book from aha! Process, Bridges to Health and Healthcare, coming out in January, deals with these timely issues.
As Breast Cancer Awareness Month comes to an end, most of us must admit to knowing something about the radical bilateral mastectomy performed on the 38-year-old Angelina Jolie last May, if only by reading magazine headlines while standing in line at the grocery store. This sensational story not only underscores the ways our healthcare system can support women—famous or not—but at a deeper level, it highlights how it can fail to provide women with the kind of informed choices that can dramatically impact their lives. A new book from aha! Process, Bridges to Health and Healthcare, coming out in January, deals with these timely issues.
Jolie’s surgery was performed by a young, committed female surgeon named Kristi Funk who established the Pink Lotus Breast Center in Beverly Hills after serving as director of the Breast Center at Cedars-Sinai in Los Angeles. Dr. Funk is described in the October issue of Town and Country Magazine as a “prototypical surgeon” for whom the inspiration for Pink Lotus came, in part, after she saw the healthcare system “routinely failing to support women” after an abnormal mammogram or a positive BRCA mutation. She recognized that “women are anxious, and no one talks to them.”
Funk’s husband, Andy, who runs the Pink Lotus Breast Center, agrees. “Cedars-Sinai and other big hospitals in Los Angeles are not designed for the patients they serve. Specialist doctors each do their own thing, and patients bounce around among them, having to make their own appointments and even carry their records from place to place. As a result, no one seems to have a plan, and nobody is in a particular rush to communicate with the patient.” He says that patients end up more worried about understanding the healthcare system than they are about the condition they are trying to get treated.
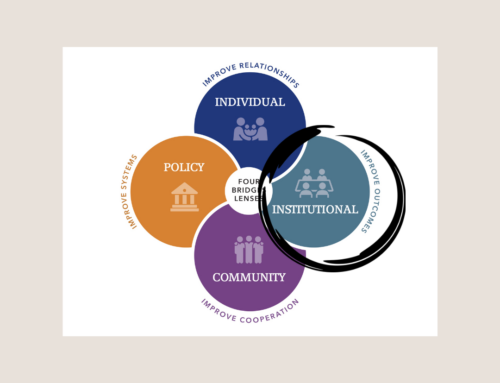
Addressing the challenge of such communication and education gaps is one of the core strategies taught in Bridges to Health and Healthcare. First, we must learn to see our clients, customers, students, and patients through the lens of economic class. Threats to health like cancer create a level playing field for all classes in terms of basic instincts for survival and emotional stability. The woman in poverty is already bombarded by issues of survival like transportation, child care, the burden of agency time and the great possibility that her resources are already unstable at best. Often the middle class or wealthy woman like Jolie will have the desire, skills, cognitive and financial resources to take on this new and very real threat to survival. Yet, what seems to be in question here is the capacity of the institution to attend to the emotional resources available for the patient– a patient who (in the moment) often lacks the ability to manage the rules, policies, papers and formal register imperatives of the healthcare entity. Then, in response, institutions must come to understand the Customer Life Cycle, which encompasses all that the customer (patient) endures before she gets to the doctor or hospital. And finally, we need to help direct what happens in those critical first 15 minutes of engagement. Is she greeted with apathy or empathy? Is she separated from human kindness by a glass partition, a computer screen and a clipboard? Is she greeted with the help of a patient navigator or advocate to direct and assist in the completion of paperwork and the answering of the questions that serve the system? Are there small social amenities that imply that the emotional trauma is understood? These may range from safe places to hold children while she is seen down to a warm cup of coffee or tea. More importantly, is she greeted and cared for in those first fifteen minutes by someone capable of viewing this experience through a common lens. Is she greeted with an attitude of possibilities for nurturing in a truly freightening situation?
Imagine applying this simple series of actions to the experience of the woman with newly diagnosed breast cancer. Overlay that with compassion and an understanding of self-, institutional-, and community efficacy, and we might be able to abort some of the confusion and pain that accompanies this dreaded diagnosis. Moreover, we may open the door to a plethora of intuitive and ingenious ways to transform care delivery systems.
To pre-order a copy of Bridges to Health and Healthcare, or to receive an email when the book is available for purchase, please email us at books@ahaprocess.com.